A full demographic breakdown of study participants is provided in Table 1. Participants in this study were predominantly Non-Hispanic White (60%), married (95%), held advanced degrees (85%), and were first-time parents (60%). The average age of participants was 34.6 years. At the time of data collection, just over half of participants were over a year postpartum and 60% self-reported having had a high-risk pregnancy.
Six women (30%) reported mild anxiety symptoms, with GAD-7 scores in the sample ranging from 0 to 9. Despite generally low symptom severity, half of the participants indicated that their symptoms made it somewhat or very difficult to do work, take care of things at home, or get along with other people. The two most reported symptoms were feeling nervous, anxiety, or on edge (n = 10) and worrying too much about different things (n = 10).
While only three women (15%) reported having mild depressive symptoms, PHQ-9 scores in the sample ranged from 0 to 6. Despite generally low symptom severity, 11 participants (55%), including those with a PHQ-9 score of 2–4, reported that their symptoms made it somewhat or very difficult to do work, take care of things at home, or get along with other people. The majority of women reported having problems feeling tired or having little energy several days (n = 12, 60%), with a subset reporting having felt this symptom more than half of the days (n = 2, 10%), or nearly every day (n = 2, 10%) over the past 2 weeks. All the women who screened positive for mild depressive symptoms also screened positive for mild anxiety.
Additionally, 12 of 20 participants agreed that COVID-19 had an effect on their mental and/or physical wellbeing. Roughly a third of participants felt other external factors negatively impacted their mental and physical health, with identified factors including political climate in the U.S., international wars, climate change, transitions to parenthood as a working parent, body image, loss of a family member, and gun violence in schools.
The following sections detail three themes generated from the interview data related to mental health and coping during pregnancy and postpartum: isolation and loneliness as a result of COVID-19 disruptions, fear and anxiety resulting from simultaneous information overload and uncertainty surrounding COVID-19, and coping mechanisms to confront stress, anxiety, and loneliness.
The COVID-19 pandemic interrupted social interactions and obstetric care resulting in isolation and feelings of loneliness
Disruptions to social interaction and community-building during pregnancy contributed to feelings of loneliness among participants. Efforts to minimize COVID-19 exposure limited opportunities to connect with friends, family, and broad support networks through events such as baby showers, resulting in a sense of detachment from usual social circles. Many participants described the loss of informal and structured avenues for maintaining social connection, and some turned to virtual forms of support as partial substitutes for in-person interaction.
I would say I felt lonely a lot of the time, and you don’t have the normal social gatherings. It was harder to see people just in general. It was incredibly lonely after having the baby because then we definitely weren’t seeing anyone. (White, 32 years old)
I think being pregnant during COVID-19 and being at home was very isolating. It was hard. I’m a very social person, very extroverted, so it felt challenging to not be able to be around people. But I have a lot of good friends that I was able to call and message and Facetime and Zoom with, especially those that had kids already and getting encouragement from them. (Asian, 33 years old)
A minority of participants did highlight how virtual contact was not wholly satisfying. The pandemic simultaneously isolated and increased fear among pregnant and postpartum people, with virtual interactions serving as imperfect substitutions.
More than half of patients, all of whom delivered by early 2021, reported that visitor restrictions for prenatal care visits made them feel lonely and deprived them of a major source of support during these clinical encounters. Several participants recounted feeling emotionally alone during critical points of their prenatal care, such as ultrasound screenings, and feeling disappointed that they could not share these moments with their partners. This was particularly true for women who experienced high-risk pregnancies, nearly all of whom reported feeling both physically and emotionally alone. At least one individual expressed that the benefits of having social support at clinical encounters outweighed the additional COVID-19 exposure risk, especially since spouses often shared the same living environment and took the same precautions to reduce exposure and spread of COVID-19. Participants with high-risk pregnancies also described their prenatal care experience as a period filled with anxiety because, at times, these individuals had to receive difficult news on their own. One participant who experienced an early miscarriage describes how painful it was to watch an ultrasound of her lost pregnancy while her partner could only support her over the phone. Another participant recounted the moment when she learned that her baby has a genetic disorder. She emphasized the emotional burden of taking in this information without her partner present and the lasting impact it had on her mental health:
But early on, after the genetic testing was done…we found out that she was going to have a high probability of having down syndrome, trisomy 21. So going through that by myself and seeing the genetic counselor, like, I wish he could have been there for that. I was reliving getting the phone call, sitting in meetings, and just thinking, ‘why do I have to retain all this information by myself when it’s emotional?’…and doing that alone was just a little more difficult. (White, 42 years old)
Another parent described how the clinical staff were not equipped to provide the necessary emotional and mental health support when recounting her experience having a miscarriage during the pandemic. She stated:
I will never forget the feeling of crying into an N95 by myself in a room because…an ultrasound tech was like, well, let me go find a provider to talk to you. So, she had to round up some random provider to talk to me about what the next steps were. (White, 36 years old)
Multiple participants expressed concern about hospital visitor restrictions forcing them to deliver in a hospital alone, however, this did not occur for any of the twenty who were interviewed; they were all permitted to have one visitor stay with them during the birth.
In the post-partum period, participants recovered and cared for their newborns in the same setting of isolation that had characterized the antenatal period. One participant described being anxious about COVID-19 exposure to her newborn and the lengths she and her partner took to protect their child:
I just would have loved to have been with all of the family and to have that community and pass the baby around or just kind of have that kind of connection. I feel like that was kind of really striking to me in terms of just the isolation. And we don’t take [my daughter] with us to go grocery shopping. We don’t take her with us to go anywhere. And so that feels unfortunate. (White, 36 years old)
The COVID-19 pandemic left participants alone in both the difficult and celebratory moments of pregnancy. The occurrence of pregnancy complications and loss, events that alone can negatively impact individuals’ mental and emotional health, were worsened by the restricted access to sources of support during earlier periods in the pandemic when stricter clinical visitation limits and social distancing measures were in place.
A sub-set of participants explicitly named that their decision to adhere closely to social isolation measures during the antenatal and postpartum periods was out of fear of COVID-19-related maternal complications. One participant severely restricted contact with her extended family members due to opposing views on the severity of COVID-19, and the fear that her family members were not taking proper precautions to prevent the spread of the virus to her and her newborn. The practice of social isolation could also be extreme for those who chose not to vaccinate and were afraid of contracting the virus. One participant, whose family chose not to vaccinate, had older children at home and started homeschooling them when in-person school returned.
Simultaneous information overload and uncertainty surrounding COVID-19 led to fear and anxiety
More than half of study participants were pregnant in the early days of the pandemic, when information about COVID-19, the vaccine, and impacts on pregnancy was emerging rapidly with interpretations of this data varying among different sources of information and among the same sources over time. In this setting of uncertainty and simultaneous information overload, participants had to make important decisions, such as whether to get the COVID-19 vaccine, or how to adhere to social isolation measures. Participants sought health-related information from physicians, public health experts, and news outlets, as well as drawing on input from friends, neighbors, and the internet.
In the early days of the pandemic, participants felt that pregnant people were left out of the public health discourse about who was at high-risk for serious complications of COVID-19. They eventually learned that being pregnant put them at higher risk of infection, and also that infection could have very serious and deadly consequences for them.
But anything specific related to COVID pregnancy I think it was so new and so early that it was a I guess you would call us a high-risk group that wasn’t really being talked about as much as people who had respiratory issues or other autoimmune issues. It was, oh, and pregnant people, but we really don’t know what’s going to happen with them or what the impact will be. (Black, 43 years old)
At the beginning, it was just kind of like we – pregnant women weren’t even considered high-risk, and then we were at, a high-risk group. So, it kind of evolved. It’s like, oh, now you’re high risk. I was like, okay, well, I’m definitely not going to grocery stores and that sort of stuff. (White, 38 years old)
What began as fear of the unknown became rooted in reality as more news about pregnant people requiring hospitalization, or even dying, came to light. Participants also expressed fear of being separated from their newborns if they tested positive at delivery. Even considering that this cohort had heavy representation from highly educated public health workers, it was common for participants to struggle to digest data related to COVID-19 and make decisions about preventing infection. Participants frequently expressed being nervous about making the right decision when surrounded by the changing tides of information.
The constantly evolving information landscape was even difficult to navigate for the health professionals who were advising participants, which put further pressure on individuals to navigate different sources of sometimes contradictory advice. One participant signed up to receive the vaccine when it was first released and said that the pharmacy administering it tried to deny her upon learning she was pregnant. She describes how she had to press hard to convince the pharmacist to give her the vaccine:
She came with the shot and was holding it and I remember it so vividly, she goes, ‘I don’t know what this can do to your baby and so I’m not sure if you should get vaccinated or not. So if something happens to your baby, then I can’t be held responsible and I want you to make sure that you actually want to do this.’ And I was sitting there and I was like, yeah – and I literally had the [American College of Obstetrics and Gynecology] report printed out and everything. I was like ready to go because I figured they were going to be a pain…She was like, ‘you’re the first [pregnant] one…I could be liable if your baby dies.’ (Hispanic, 33 years old).
In another example, one individual explains how her obstetrician changes his mind about vaccination during her prenatal care:
I talked to my [obstetrician] about [vaccination] and because he didn’t know anything about it, he was like, I don’t want you to take it…But I think he must have learned more about it because when I started to see the [maternal fetal medicine specialist] and I asked him about it again, he was like, yeah, you probably should take it. (Black, 38 years old)
Access to abundant information was described as having both negative and positive impacts for pregnant women. There was so much to take in that in some cases it was reported to cause confusion, create discord between patients and healthcare workers, and cause anxiety for pregnant women who had to make important decisions about their health. At the same time, information could also be empowering if they trusted the source and data provided.
Using multiple coping mechanisms to confront stress, anxiety, and loneliness
Approximately a quarter of participants (all first-time parents) shared that they accessed professional mental health resources during their pregnancies. Only one person self-disclosed that she had been diagnosed with generalized anxiety in pregnancy and reported accessing mental health services in the postpartum period. She expressed that the main barrier to getting mental health care at that time was the availability of mental health providers, stating “The demand for therapists is so high that just the wait times to get an appointment are huge.” Women developed their own support networks and coping mechanisms, often combining different methods in order to tend to their mental health and break up periods of isolation (see Fig. 1 for a depiction of how different combinations of coping strategies were used in this cohort). Participants described relying on virtual support groups, doula services, and prenatal classes throughout their pregnancies. They used outdoor spaces for recreation and to find a respite from isolation and stress inside the home. Many also cited their partners as a source of support during their pregnancy. Finally, women found support in their friends, extended family, and neighbors, often seeking out pregnant peers in these networks for solidarity.
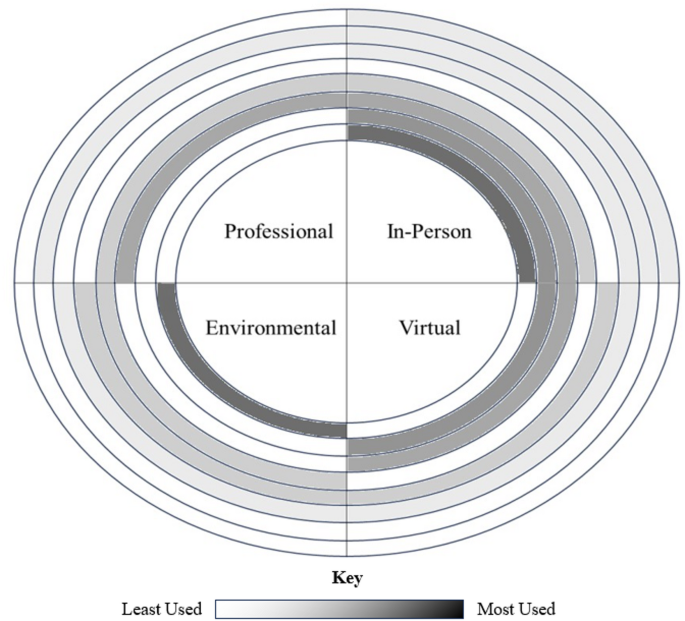
Frequency and combinations of mechanisms used to cope with stress, anxiety, and loneliness. In this figure depicts the combination of coping mechanisms used by study participants to cope with feelings of stress, anxiety, and loneliness. Reported strategies were clustered into four categories: (1) treatment by mental health professionals (i.e., Mental Health Treatment), (2) engaging in in-person interactions with people in one’s social circle (i.e., In-Person), (3) engaging in on-line interactions with people within and beyond one’s social circle (i.e., Virtual), and (4) spending time outdoors to experience a shift in environment and take comfort in natural surroundings (i.e., Environmental). Participants varied in their coping approaches, with some relying on a single strategy and others using multiple strategies across categories. There were eight reported combinations of the four types of coping mechanisms, displayed by the presence of one or more highlighted quadrant segments in each ring. Each rung illustrates which coping mechanisms co-occurred and how frequently they were used, with the most commonly reported combinations appearing in darker shading and positioned closer to the center, and less frequently reported combinations extending outward. For example, the most common pattern involved a combination of environmental and in-person coping mechanisms, whereas fewer participants reported relying solely on in-person coping mechanisms.
Online engagement was the most common way participants reported accessing support. Half of the participants mentioned that they relied on virtual support services during their pregnancies, such as Facebook mom groups, with virtual platforms also serving as a way to celebrate pregnancy.
I think outside of the health care setting, I would encourage any pregnant woman, even if you’re in the middle of a pandemic, still do those things that you wanted to do. Even if it’s going to be out of my smaller scale, if you wanted to have a gender reveal, do a virtual gender reveal, which is what I did…because it’s important to mark it. I think it just gives you strength sometimes when this can be so stressful. [Pregnancy] is definitely a physical experience, but I think the mental and the emotional and the social is critical. (Black, 33 years old)
Through technology, pregnant women could find relief from some of the loss and stress associated with isolation. On the other hand, more than half of women took to outdoor spaces for recreation and stress relief. They took up hobbies such as hiking and gardening as these were considered safe activities that bore low risk of infection.
When detailing how they coped with the stress and anxiety of being pregnant during the pandemic, women described how they drew on broad networks for support. Most credited their partners as a vital source of support, with two using their husbands as a stand in for a doula, but they also named family members, neighbors, friends, coworkers, and church members as sources of comfort. These individuals shared parenting tips over text messages, helped run errands, joined them for walks, dropped off food when checking in on them, among other things.
Two other girlfriends were pregnant with me during my first pregnancy. And we talk every day, all day on the text about how all the babies, all the spouses, how everybody is doing all the time. And they are a constant support network. (White, 34 years old)
This was in contrast to one participant who expressed not having a strong support network during pregnancy. When asked what support she felt was missing, she replied:
I wanted to be building a village, like building that community, and that didn’t get to happen. So, there was no one to call or text to be like, just with whatever with random questions or to commiserate. (White, 30 years old)
Though this individual participated in virtual support groups, she felt that speaking with strangers on the internet was not an equivalent stand in, demonstrating the limits of virtual platforms.
link

