Study design and participants
The ELSA study is an ongoing, nationally representative, longitudinal study conducted among residents older than 50 years in England to investigate a broad range of topics on ageing process13. The first wave of ELSA study was performed in 2002/03 and followed up biennially after that. Data were collected using self-completion questionnaires and computer-assisted face-to-face interviews. The collection of biological samples and examination of physical functions were performed every four years during the nurse visits. The PF was first measured at wave 2 (2004–2005) which was used as the baseline. In the present study, 14-year data from wave 2 to 9 (2018–2019, the latest wave released) were available for an association analysis. The ELSA study was ethically approved by the National Health Service Multicentre Research and Ethics Committee, who confirms that all experiments were performed in accordance with relevant guidelines and regulations. Written informed consent was provided by participants.
Gait speed was measured among participants aged 60 years and older. Among 9432 participants at baseline, we excluded individuals who were ineligible to test gait speed (age < 60 years, n = 3186), had missing data on PF (n = 1445) or MCR (n = 17), had prevalent MCR (n = 418), or had self- or proxy-reported history of dementia (n = 14). Participants who developed incident dementia at or before the visit of MCR occurrence during follow-up surveys were excluded (n = 13). We also excluded participants who had no follow-up survey (n = 665) or had missing data on covariates (n = 110) (Supplementary Figure S1). A total of 3564 participants were retained for data analysis.
Measurement of PF
The PF was tested at waves 2 and 4 in the ELSA, and we used PF at wave 2 as the exposure. The nurse applied a hand-held spirometer (Escort, Vitalograph, Bucks, UK) to examine PF indicators including forced expiratory volume in 1 s (FEV1, liters), forced vital capacity (FVC, liters), and PEF (liters per second). Participants were instructed to follow the correct method of measurement demonstrated by nurses when standing up and removing tight clothing. They completed at least three technically satisfactory exhalations, the maximum value of each PF indicator was used in this study. Raw values of the three PF indicators were converted into standardized z-scores using the mean and standard deviation at baseline. A CPF was calculated by averaging the z-scores of FEV1, FVC, and PEF, with higher values indicating better lung function9. It has been proposed that the CPF, aggregated from three indicators of FEV1, FVC, and PEF, captures comprehensive lung health because it reflects both pure PF and the contribution of respiratory muscles14.
Assessment of MCR
Individuals who had subjective cognitive complaints and slow gait were defined as having the MCR according to previous studies1,15. Gait speed at each visit and subjective cognitive complaints at waves 1–4 and 7–9 were available in the ELSA. Participants were asked “How would you rate your memory at the present time? Would you say it is excellent, very good, good, fair, or poor?” during the interview. Individuals who answered “fair” or “poor” were regarded as having subjective cognitive complaints. Participants aged 60 years and older were invited to test the gait speed. They were instructed to undergo a timed 8-feet (2.44 m) walking test at their usual walking pace twice. The average time of the two walking tests was used to estimate gait speed in feet per second. Slow gait was defined as walking speed one standard deviation (SD) below age- and sex-specific means at baseline according to the methods used in previous studies1,15. Cut-off points of slow gait by age and sex are shown in Supplementary Table S1.
Covariates at baseline
Covariates were chosen based on associations with PF and MCR according to previous studies4,9,10,15,16. During the interview, structured questionnaires were used to collect information on age (in years), sex (male or female), self-reported race (White and non-White), and educational attainment (lower than ordinary or advanced [O/A] levels, O/A level, higher than O/A level, and foreign or other). Self-reported marital status was divided into three levels of never married; separated, divorced, or widowed; and married or partnered. Smoking status contained three groups of never, current, and past smoking. Drinking levels were quantified as drinking days per week. Participants were asked how often they took mild, moderate, and vigorous activities, with prompt cards to interpret the physical activity intensities. Physical activity scores were calculated by summing up the scores of vigorous (0 for hardly ever or never, 2 for one to three times per month, 6 for once a week, and 12 for more than once a week) and moderate physical activity (scoring as half of vigorous activity), with higher scores referring to higher levels of physical activity17. Body mass index (BMI, kg/m2) was calculated as body weight divided by height squared. The 8-item Center for Epidemiological Studies-Depression scale (CES-D) was applied to assess depressive symptoms, with higher scores (0 to 8) indicating severer symptoms18. The burden of chronic conditions was assessed with the histories of self-reported doctor-diagnosed hypertension, diabetes, lung diseases, heart diseases, stroke, arthritis, and cholesterol diseases. Following a previous study19, global cognitive function was estimated by averaging the z-scores of three separate cognitive tests covering memory, orientation, and verbal fluency, with higher scores indicating better cognitive status.
Statistical analysis
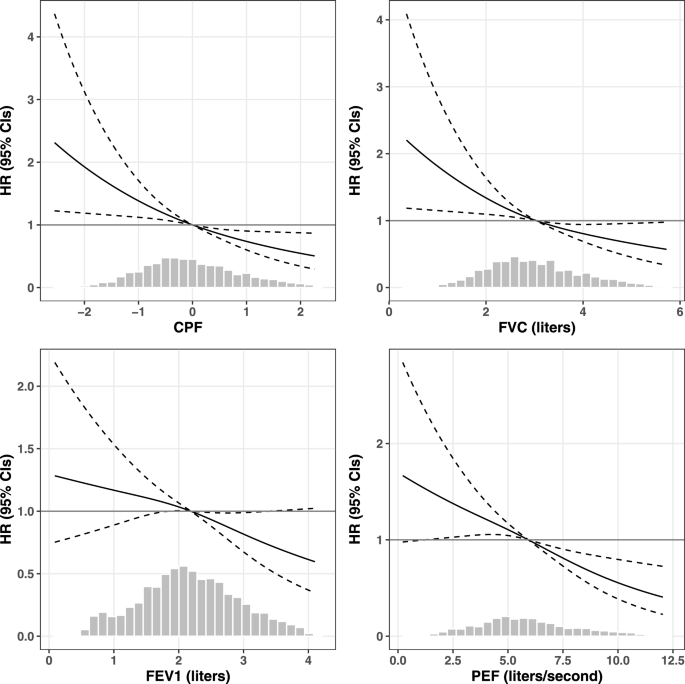
Each PF indicator was categorized into three groups of low (tertile 1), medium (tertile 2), and high (tertile 3) according to tertiles in all participants. Ranges of tertiles in all PF indicators are shown in Supplementary Table S2. Baseline characteristics of participants across CPF categories were compared with the analysis of variance for continuous variables and Chi-squared test for categorical variables. Survival time was estimated as years of follow-up interval between baseline and the occurrence of incident MCR, loss of follow-up, or the last visit (whichever came first). For participants who developed dementia without experiencing interim MCR, they were censored at the last available follow-up that showed no MCR before dementia diagnosis. Cox proportional hazards regression models were employed to examine the association between PF and MCR, adjusting for age, sex, race, and education in Model 1, and additionally adjusting for marital status, smoking, drinking, physical activity, BMI, CES-D scores, history of chronic conditions, and cognitive function in Model 2. The proportional hazards assumption was tested with the method of scaled Schoenfeld residuals. PF indicators in continuous and categorical values were separately analyzed. The R package “rms” was applied to examine potential nonlinear relationships between PF and MCR using restricted cubic splines with three, four, and five knots. We selected three knots as the optimal parameter due to its minimum value of Bayesian Information Criterion. The potential nonlinearity in PF-MCR association was tested with the method of Wald test.
Sensitivity analyses were performed when using PF indicators divided by height squared to adjust for body size20, and when applying weighted Cox proportional hazards regression models in consideration of the complex sampling design21, as well as using the inverse probability weighting for Cox proportional hazards regression models to adjust for the selection bias caused by the loss of follow-up. A sensitivity analysis was also conducted by removing participants with a possible chronic obstructive pulmonary disease (COPD) which was defined as a FEV1/FVC ratio of less than 0.79. Besides, the follow-up time was calculated when using the midpoint between the last visit without MCR and the first visit with MCR as the onset of incident MCR in consideration of the interval censoring limitation.
All data analyses were performed with R, version 4.2.1. A two-sided P value less than 0.05 indicated statistically significant.
link